Public Health Emergency of International Concern: the Zika Case
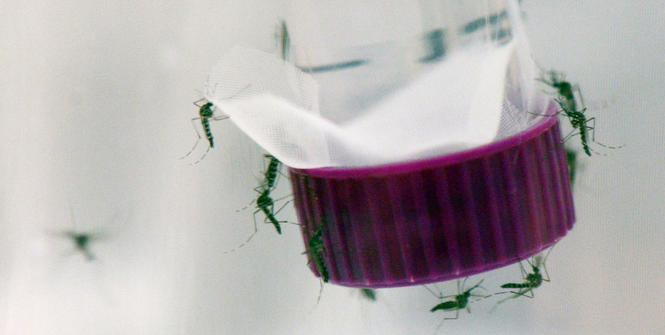
Two confirmed cases of the Zika virus have been detected in Australia, just two days after the World Health Organization (WHO) declared the Zika outbreak in Central and South America to be a “Public Health Emergency of International Concern” (PHEIC).
The Zika virus is usually a mild mosquito-borne illness that causes flu-like symptoms. It is spread by the Aedes africanus and Aedes aegypti mosquitoes found in Africa and Asia. In 2007, 2013 and now 2015, the virus has moved to new locations: Yap Island, Pacific Islands and now South America (respectively).
The 2013 outbreaks in French Polynesia were linked to higher than usual caseload of nervous disorders and now also, in 2015, microcephaly (brain damage in infants at birth) in South America. The decision to declare the Zika outbreak a PHEIC, at this time, is correct and momentous for three reasons.
Added value
Up until now, there has been concern, confusion and apparent reluctance to regularise the use of the International Health Regulations (IHR) notification and decision instrument to discuss events that may constitute a PHEIC. Under the revised IHR (2005) there are three “events” that should inform the declaration of a PHEIC: the outbreak of an unknown pathogen, the outbreak of a listed disease in the IHR assessment and notification instrument algorithm, or an outbreak event with the potential to become a PHEIC.
As the Chair of the IHR Emergency Committee on Zika, Dr David L. Heymann has noted, Zika itself is a mild disease, but if it is causing microcephaly in infants and nervous disorders in adults then it has the potential to become a PHEIC.
The “added value” of WHO declaring this mild, mosquito-borne illness a PHEIC is that this was what IHR was designed to do: compel cooperation and information sharing amongst states, encourage states to promptly report outbreak events, and permit the WHO to coordinate the information and research necessary to determine the link between Zika and grave illnesses such as microcephaly and Guillain-Barré syndrome.
Institutional reform within WHO
The WHO has demonstrated the capacity for adaptation despite its institutional limitations. In 2015, there was widespread alarm and condemnation at the WHO’s reluctance to convene an IHR Emergency Committee to discuss the Ebola outbreak in (primarily) three West African countries: Guinea, Liberia and Sierra Leone. It took five months between the first notification of confirmed Ebola cases in March 2015 and the Committee being convened in July 2015. Over 20,000 people died from this disease and it challenged even the humanitarian organisations with a history of responding to humanitarian crises, such as MSF.
Since then, there have been a series of scathing reports – including internal reports – describing the organisation as slow to react to public crises and reluctant to engage with other UN agencies and to communicate decision-making processes. Arguably, Dr Margaret Chan, WHO Director-General, cannot be accused of responding slowly to the Zika virus if you examine at the timeline of events.
The Brazilian government announced a possible link between Zika infection and microcephaly in infants in October 2015. The WHO and its the regional office – Pan American Health Office (PAHO) – issued an alert on 17 November calling for all states to investigate potential links between Zika infection and microcephaly. In January 2016, Brazil government announced it was investigating at least 4000 suspected cases of microcephaly, as well as higher than average cases of Guillain–Barré syndrome.
A call for support
Finally, the declaration of PHEIC is not a punishment or indictment on the behaviour state(s) affected by the outbreak. The consensus has been that Central and South America states have followed Brazil’s example and been open about their caseload, their surveillance capacities and their shortfalls in response. The IHR is not a reprimand but a call for support to affected states, assistance with research and development and attention on the crisis.
The IHR has a history of being an instrument that lacked “authority”. The revisions in 2005 were aimed at modernising the alert instrument, improving cooperation in outbreak response between states and the WHO, as well as improving national capacities to track, report and respond to an outbreak event.
Of course, there was and remains a desire for states to report early and often in order to permit the international community time to prepare for outbreak events. However, “unnecessary” (under the terms of the IHR) trade and travel measures by some countries against countries with high cases of H1N1 (“Swine Flu”) in 2009, followed by similar responses again during the Ebola cases in 2015, risked confusing the purpose and value of the IHR and declaring a PHEIC. The Zika PHEIC declaration clearly states travel and trade restrictions are unnecessary. This captures the spirit and intention of the revised IHR.
What’s next?
Similar to the Ebola outbreak, there are outstanding questions about the sustainability of outbreak response in a situation where disasters, whether natural or man-made are on the rise. There are institutional questions about the cases that have not been declared a PHEIC (and why), such as the Middle East Respiratory Syndrome (MERS) – with cases continuing to occur across Middle East and Asia. There are rights and equity questions to be answered about the denial of sexual and reproductive rights in Central and South American countries where women are now being told not to become pregnant for two years. Specific to Zika, the issue is how to address the unpredictable virus.
Mosquito-borne viruses are not new to South America. In fact, the difficulty in detecting Zika and controlling it is a similar story for Dengue, Yellow Fever and Chikungunya – present across the Southern Hemisphere and all considered, until now, more serious than Zika. But there are broader lessons to be learnt about this outbreak that go beyond the WHO issuing a PHEIC: namely, the right to a national health system that can conduct provincial-level surveillance to detect unusual health events and respond appropriately. These are costly structures but it may have saved Brazil from an even greater cost to its economy. For all the hype about twitter alerts and event data detection, it was the national public health sector that detected and reported the unusual spike in microcephaly and Guillain–Barré cases.
This was precisely the argument made with Ebola, and before that, H1N1, H5N1 and SARS. This why we are seeing renewed engagement and discussion on universal health care coverage in the UN General Assembly and World Bank. Crucially, some of the countries strengthening their health systems are the ones we have collectively depended on to track Zika, Ebola and other emerging pathogens in recent history: Argentina, Brazil, Chile, China, Columbia, Costa Rica, Ethiopia, Georgia, Ghana, Guatemala, India, Indonesia, Jamaica, Kenya, Kyrgyz Republic, Mexico, Nigeria, Peru, Philippines, South Africa, Thailand, Tunisia, Turkey and Vietnam.
A public health system with universal health care coverage will not stop the inevitable but it will detect, respond and alert faster than any other early warning system. There are exciting and important developments that must be financially supported and replicated across regions.
Dr Sara Davies is an Australian Research Council Future Fellow and Associate Professor, Centre for Governance and Public Policy, School of Government and International Relations, Griffith University. She is also an Adjunct Associate Professor, School of Social Sciences, Monash University. This article may be republished under a Creative Commons License.





